|
By Melody Curtiss, HCW Executive Director When Mercy Hospital's operating suite opened, Project Cure, through a generous donor, provided a large donation of medical equipment to outfit the new suite. Unfortunately, a surgical table, a very expensive and essential piece of equipment, was not available in Project Cure's warehouse at that time. For the time being, the Mercy surgical team would have to make do without a surgical table. Missioners Dr. Gary Gilkeson and his wife and HCW board member Mary Ann Gilkeson had connected HCW with the Medical University of South Carolina (MUSC) to discuss global health outreach to Africa, and we were stunned and blessed to discover MUSC's enthusiasm, immediate connection to our cause, and their desire to be of assistance. MUSC's Dr. Beth Gray and Dr. Misti Leyva traveled to Sierra Leone with the Gilkesons to collabroate with the Mercy staff. They carried over equipment in their luggage, worked with the medical staff to identify needs they could fulfill, and were planning to return in July 2020 when COVID shut everything down. (You can read more about the Gilkesons and MUSC's involvement in our Summer 2020 Magazine, "Not in my wildest dreams" page 12) MUSC generously offered to let Kim Nabieu, the Gilkesons, and me roam through their warehouse of surplus medical equipment in Charleston. Miraculously, Kim and Dr. Gilkeson spied a surgical table in the corner of the warehouse. Imagine our delight when MUSC agreed to not only donate the table, but also to store it until it could be shipped, and assist with the crating! With those matters resolved, we faced a new hurdle. The difficulty was trying to get the bed to Sierra Leone, both in terms of logistics and cost. It took 18 months, miraculous interventions of generous donors to provide for the cost of shipping, and the determination of the Gilkesons, the MUSC staff, and our partner church Bethel UMC, to get the bed from Charleston to Bo. After a year of further delays and complications with the shipping company, HCW's Program Finance Specialist Cynthia Grant (who is also M&E Team Lead and an international negotiation mastermind) was able to team up with Catherine Norman, the UMC Health Coordinator in Sierra Leone, to get the surgical bed to its destination, where it will enable the Mercy surgical staff to perform surgeries and save lives.
0 Comments
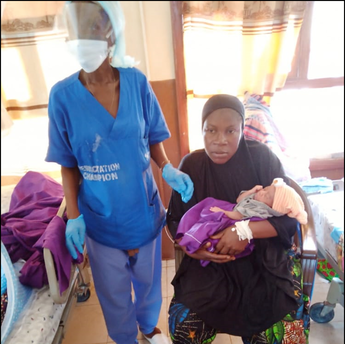 Kadiatu's pregnancy was near term when she came to the hospital with severe complications, including appendicitis, umbilical hernia, and ovarian cyst, endangering both her life and that of her baby. The Mercy surgical team quickly delivered the baby, a healthy baby girl, and subsequently performed an appendectomy, cystectomy, and hernia repair on the mother. Mom Kadiatu received a transfusion from Mercy's blood bank and after a brief hospital stay, was released in good condition. The emergency surgery almost certainly saved the life of both Kadiatu and her precious baby girl.  Josephine came to the hospital in non-productive labor, and an examination revealed that the baby was in distress. An emergency c-section was performed, and the team discovered that the baby's umbilical cord was wrapped around her neck. The baby was quickly freed and began crying without needing resuscitation. Josephine and her beautiful baby girl were discharged in good health. The maternal mortality rate in Sierra Leone has long been one of the highest in the world, with maternal deaths accounting for more than 30% of all deaths amongst women aged 15-49 years (https://www.unicef.org/sierraleone/maternal-neonatal-and-child-health.) The leading causes of maternal mortality in Sierra Leone are obstetric hemorrhage, hypertension, obstructed labor and sepsis. One of Mercy Hospital's primary objectives is to radically improve maternal and infant survival, and the ability to perform emergency surgery is a key provision in achieving the goal.
|
Follow us on social media
Archive
July 2024
Click the button to read heartfelt tributes to a beloved Bishop, co- founder of our mission!
Post
|
Helping Children Worldwide is a 501 (c) 3 nonprofit organization | 703-793-9521 | [email protected]
©2017 - 2021 Helping Children Worldwide
All donations in the United States are tax-deductible in full or part. | Donor and Privacy Policy
©2017 - 2021 Helping Children Worldwide
All donations in the United States are tax-deductible in full or part. | Donor and Privacy Policy