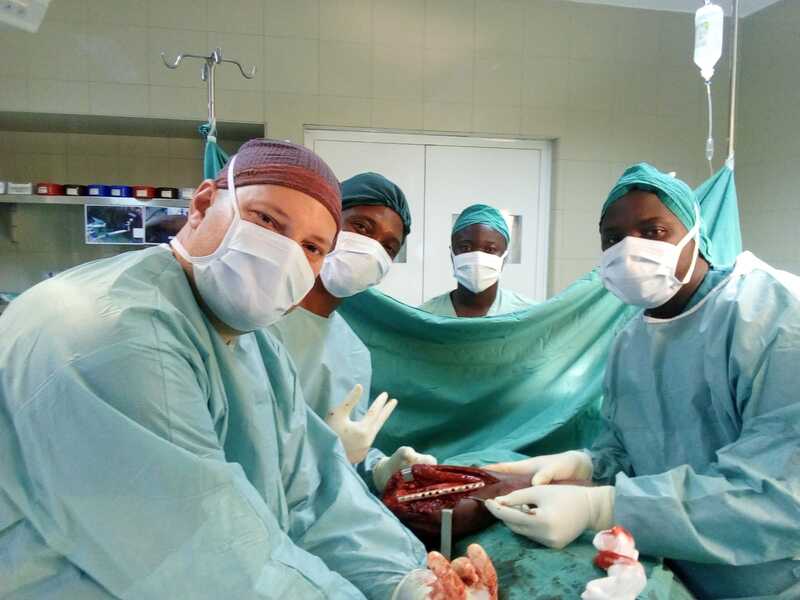
When Bishop John Yambasu tragically died in a traffic accident in August of this year, he left behind an epic legacy of love and service, but he also left a huge hole in the hearts of the many people he led and inspired. The Child Reintegration, Mercy Hospital, and Missionary Training Centre staff members have been especially devastated by his loss. They decided to hold a very special ceremony to honor the bishop and reignite their commitment to his ministry of transforming the lives of vulnerable children and families in Sierra Leone. The ceremony, called "Carry the Light" was held on September 29th at the CRC and included all staff members from the CRC, Mercy and the MTC. At the event, one big candle represented the Bishop's light, and each staff member lit an individual candle from that light, symbolizing the continuation of the bishop's vision and mission. The staff members took the candles home, so that they will continue to be a visible memento of the CRC and Mercy staff members' recommitment to their mission.
0 Comments
 Mercy Hospital is pleased to welcome Dr. Aruna Stevens to the staff. Aruna is an original alumnus of the Child Reintegration Centre residential program who was rescued from the Bo street as a small child in the wake of the Sierra Leone civil war. Aruna graduated from the University of Sierra Leone College of Medical and Allied Health Sciences and completed his housemanship (residency) at the University of Sierra Leone Teaching Hospital Complex. "Today is a start of a childhood dream that I had to be a doctor to serve people, but specifically my people of Bo and its environs. I'm very humbled for this opportunity and grateful to Helping Children Worldwide, the Child Reintegration Centre, the United Methodist Church Sierra Leone Conference, and Mercy Hospital," Aruna says.  Mercy Hospital surgical staff performed a c-section on Mabel to deliver a healthy baby girl. Mercy Hospital surgical staff performed a c-section on Mabel to deliver a healthy baby girl. Cesarean section deliveries save lives The busy Mercy staff continues to deliver babies, through normal deliveries and cesarean deliveries when necessary. Since the operating suite opened in 2018, the hospital has been able to provide life-saving emergency c-section procedures, saving the lives of mothers who are not able to deliver vaginally. The need for cesarean sections can be aggravated by a range of issues such as delays in accessing the appropriate level of care, and transportation delays. Sierra Leone has one of the highest maternal mortality ratios in the world, with 11 mothers dying of pregnancy-related complications for every 1000 live born babies. The ability to perform c-section procedures at Mercy Hospital is a critical element of the global movement to reduce maternal mortality. 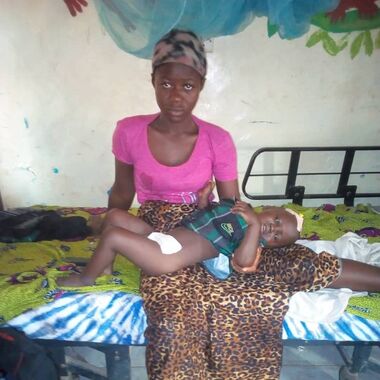 Saidu's mother comforts him after surgery to correct an inguinal hernia. Saidu's mother comforts him after surgery to correct an inguinal hernia. Simple hernia procedures save the lives of babies and toddlers Two-year-old Saidu's family brought him to the hospital suffering from an inguinal hernia, a condition that Mercy sees very often, possibly due to premature birth. Untreated, inguinal hernia can lead to permanent intestinal damage. Successful surgery was performed on Saidu to correct the hernia. His family couldn't afford to pay for the life-saving procedure for their son, and were grateful for Mercy's excellent care, which was provided for free. Inguinal hernias look like a bulge or swelling in the groin or scrotum, and may be seen more easily when the baby cries. A hernia can develop in the first few months after a baby is born. It happens because of a weakness in the abdominal muscles. To correct the hernia, the surgeon puts the loop of intestine back into the abdominal area and stitches the muscles together. |
Follow us on social media
Archive
July 2024
Click the button to read heartfelt tributes to a beloved Bishop, co- founder of our mission!
Post
|
Helping Children Worldwide is a 501 (c) 3 nonprofit organization | 703-793-9521 | [email protected]
©2017 - 2021 Helping Children Worldwide
All donations in the United States are tax-deductible in full or part. | Donor and Privacy Policy
©2017 - 2021 Helping Children Worldwide
All donations in the United States are tax-deductible in full or part. | Donor and Privacy Policy