|
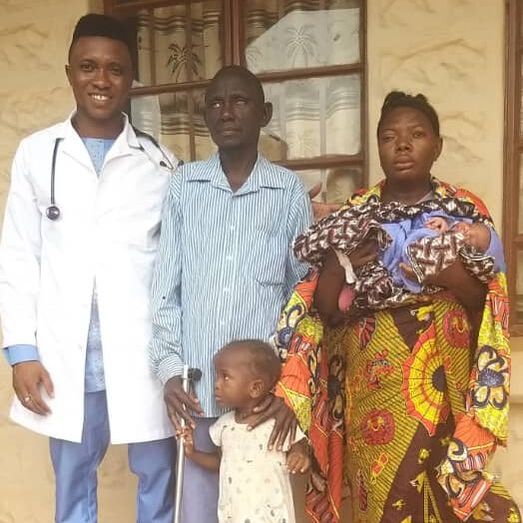
Fatmata is a very brave little two year old who helps her blind parents navigate the streets of Bo. When her pregnant mother went into labor, Fatmata guided her to Mercy Hospital to give birth. The staff delivered Fatmata's baby brother by vacuum aspiration. The family is doing well, and is deeply grateful for Mercy's timely intervention. Dr. Aruna, the attending physician, is pictured below with Fatmata, her parents, and new baby brother.
0 Comments
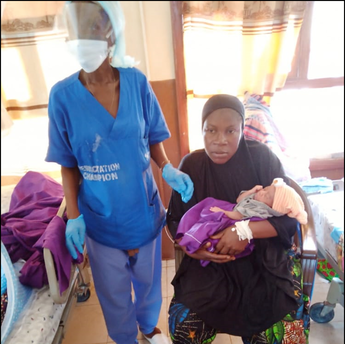 Kadiatu's pregnancy was near term when she came to the hospital with severe complications, including appendicitis, umbilical hernia, and ovarian cyst, endangering both her life and that of her baby. The Mercy surgical team quickly delivered the baby, a healthy baby girl, and subsequently performed an appendectomy, cystectomy, and hernia repair on the mother. Mom Kadiatu received a transfusion from Mercy's blood bank and after a brief hospital stay, was released in good condition. The emergency surgery almost certainly saved the life of both Kadiatu and her precious baby girl.  Josephine came to the hospital in non-productive labor, and an examination revealed that the baby was in distress. An emergency c-section was performed, and the team discovered that the baby's umbilical cord was wrapped around her neck. The baby was quickly freed and began crying without needing resuscitation. Josephine and her beautiful baby girl were discharged in good health. The maternal mortality rate in Sierra Leone has long been one of the highest in the world, with maternal deaths accounting for more than 30% of all deaths amongst women aged 15-49 years (https://www.unicef.org/sierraleone/maternal-neonatal-and-child-health.) The leading causes of maternal mortality in Sierra Leone are obstetric hemorrhage, hypertension, obstructed labor and sepsis. One of Mercy Hospital's primary objectives is to radically improve maternal and infant survival, and the ability to perform emergency surgery is a key provision in achieving the goal.
|
Follow us on social media
Archive
July 2024
Click the button to read heartfelt tributes to a beloved Bishop, co- founder of our mission!
Post
|
Helping Children Worldwide is a 501 (c) 3 nonprofit organization | 703-793-9521 | [email protected]
©2017 - 2021 Helping Children Worldwide
All donations in the United States are tax-deductible in full or part. | Donor and Privacy Policy
©2017 - 2021 Helping Children Worldwide
All donations in the United States are tax-deductible in full or part. | Donor and Privacy Policy