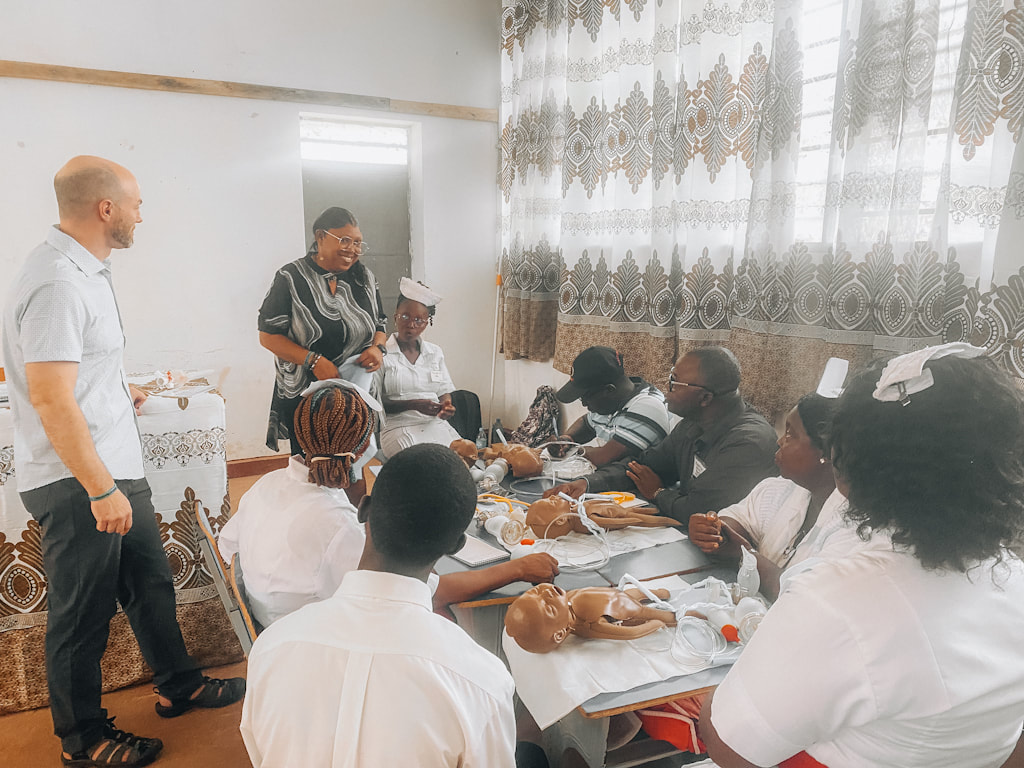Progress and Challenges in Maternal and Child Health – A Spotlight on Sierra Leone's Journey1/26/2024 Worldwide, maternal mortality is one of the most important metrics measured by the World Healthcare Organization. A country's maternal mortality reflects its capacity to care for its most vulnerable citizens– expected mothers and children–and reflects inequalities in access to quality health services. The death of a mother can have profound economic impacts on a family, as mothers contribute substantially to household income. The loss of income combined with funeral costs can severely impact a family's ability to sustain and thrive economically. Children whose mothers die in childbirth have a higher risk of dying before the age of five and are vulnerable to child marriage, malnutrition, and decreased access to education opportunities. Over the last 20 years, through the work of the Ministry of Health and Sanitation in Sierra Leone and local hospitals and clinics, maternal mortality in Sierra Leone has dropped 74%. Sierra Leone now has a lower rate of maternal mortality than the West Africa region as a whole. What used to be the deadliest place in the world to give birth is no longer even in the top ten countries with the highest mortality ratio. However, the work is not done yet. Though Sierra Leone has made remarkable progress in reducing the maternal mortality ratio, the maternal mortality ratio is still six times higher than the goal set by the Sustainable Development Goals which aim for a reduction in the maternal mortality ratio to less than 70 per 100 000 births. This means that 1 in 34 women in Sierra Leone has a lifetime risk of dying in pregnancy or childbirth. To learn more about maternal and child health mortality, check out our podcast episodes with the Child Health Mortality Prevention Surveillance Program, our Rising Tides Conference episode, and our first episode on Global Health. The leading causes of maternal death in Sierra Leone are obstetric hemorrhage, hypertension, obstructed labor, and sepsis. These are all preventable causes of death, but they are often deadly in Sierra Leone due to a lack of access to quality healthcare. If maternal mortality is a measure of the strength of a health system, then efforts to strengthen health systems can improve maternal mortality and ensure that no woman dies bringing life into the world. With our desire to do more work in health system strengthening, HCW is putting on a 5-day Maternal and Child Health Conference at Njala University in Bo, Sierra Leone. Approximately 100 midwives, nurses, and CHOs from around the Bo district gathered together this week at the Paramedical School at Njala University to learn critical practices and procedures in maternal and child health. Our primary goal is not just to improve the competence but also the confidence of 100 midwives who provide care to women during pregnancy and childbirth. Our secondary goal with this project was to bring together organizations, facilities, and individuals so we can work together in synchrony, not solitude. So, we cannot talk about the impact that this program is having on the education of nurses and midwives without talking about all the people who worked to make it happen. In the global health world, working in partnership is key to successful projects. Each of the organizations in this project has brought their own resources, networks, knowledge, and creativity to make this conference happen. We are so proud of our network partners and want to share a little about the contributions they made to this conference. Mariama Massaquoi, Executive Director at Tenki for Born, and Josephine Garnem the Executive Director at Healey International Relief Foundation, met with us at Helping Children Worldwide almost two years ago. They were already members of the Together for Global Health network, but we had never met in person before. Through the discussion, Josephine asked if we would be interested in doing a joint mission to Sierra Leone. That is how this project began, and it grew exponentially from there. Both Mariama and Josephine are featured on the latest episode of our HCW podcast talking about this conference. As we began planning the conference and training, we reached out to the Christian Health Association of Sierra Leone (CHASL), who had trained a cohort of nurses in September 2023 to see if she would be interested working with us to follow up on this training. Florence Bull, their president, was overjoyed at the idea of a partnership because it aligned seamlessly with our CCIH Health System Strengthening commitment. Tenki for Born took the lead on preparing the curriculum because Mariama is a Family Medicine Physician with expertise in obstetrics. They also purchased the simulators from Laerdal Medical. Healey’s work brought us many of the supplies needed for the training, as they specialize in shipping and procuring medical supplies. And CHASL brought the participants, leveraging their connections to faith-based institutions and the Ministry of Health. With these organizations on board, we began recruiting trainers to teach the curriculum. Tenki for Born recruited two additional staff in addition to Mariama to teach the coursework on Post-Partum Hemorrhage. They also purchased the simulators from Laerdal Medical. CHASL recruited master trainers from across the country to help teach the coursework in Helping Babies Breathe in their native language and culture. Healey leveraged their relationship with Embrace International to send 5 midwives from Canada to teach, as well as two trainers from SEED Global Health. And we at HCW reached out to our Together for Global Health network to get a neonatologist who works with Mission of Hope Rotifunk, 2 trainers from the Child Health and Mortality Prevention Surveillance program (CHAMPS), and a Sierra Leonean Administration from Midwives for Haiti to teach. This team brought a diverse mix of Sierra Leoneans, diaspora members, and longtime health care providers but first-time travelers, allowing each group to learn from one another and complement each other’s strengths.
Of course, none of this would have been possible without other organizations making financial contributions to our cause. IMG, Friends of Sierra Leone, and CHAMPS all believed in the power of this mission, and we sincerely appreciate their financial commitment to paving the way for improved healthcare for mothers and families. Supplies, curriculum, and in-kind donations were all provided by Project Hope, SOS Health and Hope, Direct Relief, Poly Care Medical, MAP International, MedShare, Brother’s Brother Foundation, JPHEIGO, and Njala University. Lastly, we want to thank the Together for Global Health network partners Rural Healthcare Initiative, Mission of Hope Rotifunk, Miracle of Help, and Better Lives Foundation for underwriting the cost of their participants to attend the training. Empowering nurses in low-income countries with expert training is not just a noble cause, it's a lifeline. Each skillfully guided pregnancy, each expertly delivered newborn, each mother returning home healthy to her family – these are the ripples of impact that stretch far beyond the conference walls. The impact of this training and the collaboration of these organizations in global health weave a stronger fabric of support, paving the way for a healthier future for all. This conference was merely the first chapter in our work of expanding our reach beyond Mercy Hospital, so we can do more to bring about a future where every expectant mother in every corner of the world has access to the skilled care of a well-trained nurse. That is the future we strive for, the future we relentlessly work towards, one nurse, one community, one conference at a time. Because for us, the journey to improve maternal health is not a sprint, it's a marathon, and we're just getting warmed up.
0 Comments
Your comment will be posted after it is approved.
Leave a Reply. |
Follow us on social media
Archive
July 2024
Click the button to read heartfelt tributes to a beloved Bishop, co- founder of our mission!
Post
|
Helping Children Worldwide is a 501 (c) 3 nonprofit organization | 703-793-9521 | [email protected]
©2017 - 2021 Helping Children Worldwide
All donations in the United States are tax-deductible in full or part. | Donor and Privacy Policy
©2017 - 2021 Helping Children Worldwide
All donations in the United States are tax-deductible in full or part. | Donor and Privacy Policy